Boy Feeds Sheep, Contracts a Viral Illness ‘With Parallels to COVID-19’
What is orf? It’s your body telling you to leave sheep the hell alone. Case in point: A 15-year-old boy contracted the viral zoonotic illness (meaning that it’s transmissible from animals to humans), likely after feeding sheep at his family farm in Conwy, a town in Wales.
“He felt as if his hands and feet were on fire,” said Brychan Edwards’ mom. “It looked like he’d been burnt all over.”
Brychan was admitted for emergency care and spent four nights and five days in the hospital. Hospital staff reportedly struggled to pinpoint the cause of the boil-like welts that covered his body, eventually determining that it was orf—a viral illness that can be passed from sheep to humans. It may have given Edwards’ physicians a run for their money, but farmers are all too familiar with it. Humans infected with orf often develop red, raised skin lesions, like the ones seen above on Brychan’s hand.
Orf is a “virus with parallels to COVID-19,” multiple news outlets reported. Bats and pangolins have been suspected of being the novel coronavirus’s reservoir species—COVID-19 has even been referred to as “the revenge of the pangolin.” But clearly, leaving only exotic animals like bats and pangolins alone won’t prevent the spread of zoonotic viruses.
“Domesticated mammals—including cats and dogs, pigs and cattle, horses and sheep—host 50% of the viruses that can be passed to mankind, despite representing only 12 species,” CNN reported.
Orf is just one example of the many zoonotic diseases that can result from rearing sheep for wool or meat:
Rabies
Like orf, rabies is a viral infection that can be passed from other mammals, including sheep, to humans. Although many associate rabies with bites, the deadly disease can be transmitted via direct contact with saliva, mucous membranes, or blood. Symptoms include headache, fever, hallucinations, hydrophobia (fear of water), and insomnia. Rabies in unvaccinated humans is almost always fatal.
Q Fever
A bacterial zoonotic disease, Q fever (aka “query fever”) is most related to ruminants, such as sheep and goats, and can be transmitted to anyone who has contact with animals infected with Q fever bacteria. Slaughterhouse workers and farmers who rear animals to send to slaughterhouses are among those most at risk of being exposed.
Inhaling dust that contains Q fever bacteria and touching milk from an animal infected with the disease are two of the ways it’s most commonly spread. However, multiple outbreaks of Q fever have occurred simply because infected sheep walked through town or wind carried contaminated matter off. Living close to a sheep farm could be enough to catch the disease. Flu-like symptoms are the most common indicators of Q fever, and the disease can cause stillbirth and miscarriage in pregnant women. Q fever can be deadly, and no vaccines for it are approved in the U.S.
Chlamydiosis
Chlamydi-what? Ovine chlamydiosis is typically contracted by humans through direct contact with birthing tissue of infected animals. According to one report, “If infected, in most humans it leads to a mild flu-like disease, but in pregnant women it can cause a severe life-threatening disease in the mother and lead to stillbirth or miscarriage of the unborn child.”
Woolsorters’ Disease
Anthrax (aka “malignant edema” or “woolsorters’ disease”) affects those who touch contaminated animal-derived products like wool (e.g., the bacteria enters an open wound), inhale the spores of the bacteria, or eat infected meat. People who work in wool mills, slaughterhouses, and tanneries are among those most at risk—Bangladesh, China, India, and South Africa are the countries with the greatest number of people susceptible to the disease. Just like all types of anthrax, woolsorters’ disease is potentially fatal.
Ringworm
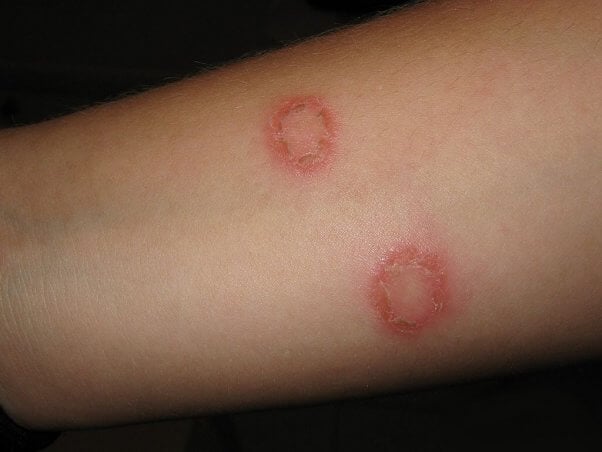
Many people who have dogs are cautiously aware of ringworm—but did you know that the fungal infection can be transmitted from sheep to humans, too? Anyone who has had direct contact with the spores on an infected animal can become infected. The spores can be on the infected animal’s wool or skin and can even be found on the brushes or clippers used to shear sheep. If infected with ringworm, humans may develop itchy, inflamed spots that appear red and scaly and will sometimes blister.
The zoonotic diseases mentioned above are only a few of the ones that can be passed from sheep to humans. Humans who have contact with sheep can also contract leptospirosis, campylobacteriosis, listeriosis, salmonellosis, tularemia, and Caseous lymphadenitis.
These sheep-associated zoonotic diseases make our wool exposés extra-disturbing.
We’ve released 13 exposés of more than 100 sheep operations across four continents, including North America, that have revealed that sheep are systemically beaten, kicked, punched, and mutilated in the wool industry. In 2018, one eyewitness who worked on a sheep farm in Victoria, Australia—the world’s top wool exporter—observed workers using shears to cut chunks of flesh off the hindquarters of lambs (i.e., baby sheep, who form deep bonds with their mothers), leaving them with exposed, bloody wounds that often become infected.
In light of the novel coronavirus crisis, we should all avoid wool for reasons beyond the important one of having compassion for sheep (who wag their tails when they’re happy, just like our canine best friends): If you buy wool, you could be fueling the next pandemic. Raising and killing sheep for sweaters, scarves, and meat can increase the risk of outbreaks of dangerous illnesses like the ones mentioned above—or even create an opportunity for new mutated viruses and bacteria to form and spread. The best way to help sheep and yourself is to refuse to buy wool.
Once you’ve clicked above and taken action, be sure to share this page with your friends and family on social media. Let them know that wearing wool—like wearing fur, leather, down, exotic skins, and every other animal-derived material—is cruel and dangerous.

